Obstacles to Routine Immunization in Madagascar: Structural, Relational and Cultural Constraints
Pasteur Institute of Madagascar - IPM (Ramaroson, Mattern, Brazy-Nancy, Ranaivoharimina); Montreal University (Ramaroson); Catholic University of Louvain (Huysmans); Catholic Relief Services - CRS (Hobisandratra, Razafiarimanana); French National Research Institute for Sustainable Development - Ceped (Pourette)
"The relationship of the populations with the health structures and healthcare personnel appears to be an essential factor in the parents' attitude to vaccines..."
Qualitative studies on immunisation in the African continent show that behaviour with respect to immunisation varies from one country to another and is multifactorial in origin. As of 2021, vaccine coverage for routine vaccines in Madagascar was low (37.8%); one explanation is the low involvement of community agents in immunisation awareness-raising activities. This article provides an overview of the individual and collective reasons leading to low vaccine coverage in Madagascar via a description of knowledge and perceptions of routine vaccine practices in children under 5 years of age.
The article presents the results from 3 qualitative studies conducted between 2016 and 2019: 2 studies conducted by the SaSS (Health & Social Sciences) team of the Epidemiology and Clinical Research Unit of IPM (Madagascar Pasteur Institute), and a Master's thesis. These anthropological studies describe practices and perceptions of childhood care, including social representations and childhood vaccine practices. These 3 studies took place in 5 different geographical areas of the island: Antsohihy (North), Manakara (South-east), Moramanga rural (East), Moramanga rural (East), and Morondava (West).
Key results:
- Mothers' knowledge about immunisation: In all 5 zones, children's health is women's business. Therefore, the mother is responsible for complying with the immunisation schedule by taking the child for immunisation. It is also the mother who knows where the health passport (carnet de santé) is kept, if it is not lost. Other women of the family (especially grandmothers) have a role in ensuring continuity of child care if the mother is temporarily not available. Despite the more frequent exposure of the mothers to messages and awareness-raising about immunisation, in all zones, the results show that the mothers have little knowledge about immunisation. More specifically, the nature of vaccines is not well understood: vaccine-preventable diseases (VPDs), single dose and multidose vaccines, mass and routine immunisations. For example, vaccines administered during immunisation campaigns appear useless for parents because they are repeated. This representation of mass immunisations fuels the belief that campaigns are politically motivated, reinforcing rumours about vaccines, such as that they could make the child sterile. The persistence of these rumours leads to the mistrust of community workers and other persons in charge of awareness-raising and vaccine administration during mass campaigns.
- What the use of the health passport reveals about the relationship with immunisation: The health passport, given by the health professional to the parents at the time of the child's first immunisation, is theoretically used to record the vaccines administered to the child and the date of the next immunisation appointments. It also contains useful information for the mothers and gives access to treatment and consultations in health centres when the child is ill. The predominance given to meeting the requirements of other activities outlined in the passport, to the detriment of immunisation, indicates that immunisation at birth is not a priority for many parents of newborn infants. (See the "Obstacles" section, below, for reasons.) Yet the presentation of a "fully completed" health passport ensures a better reception from healthcare personnel, according to parents. In the 5 zones, the women complained that if the passport is lost or damaged, the healthcare personnel scold them and can refuse access to consultations or to immunisation sessions.
- Obstacles to immunisation: In general, total refusal of immunization was not apparent from these studies. There was rather a delay or refusal of some vaccines caused by structural, contextual, or geographic obstacles:
- Structural obstacles - 2 of the studies revealed structural difficulties including availability of human resources in the health services for the administration of vaccines, availability and accessibility of vaccines, and problems linked to the open vial policy.
- Mifana and shame (a socio-cultural environment hostile to compliance with the immunisation schedule) - The findings reveal local contexts that can impede immunisation: the practice of mifana or confinement after childbirth due to the perception of the newborn as fragile, the perceived vulnerability of the young infant at birth, and the mothers being made to feel inferior/humiliated by the healthcare personnel in the health centres due to their "slovenly" clothing and physical appearance.
- Geographic obstacles - 2 of the studies show that geographic remoteness is an issue in the choice to not vaccinate the child, but closer examination of the narratives of seeking care for children and the analysis of the available care options in a limited therapeutic area (NeoVac) indicates that, when they feel the necessity, distance is no longer an obstacle. Moreover, the findings of the studies also report the fact that delivery in a health centre does not guarantee systematic immunisation of the child at birth, although in this case the geographic distance would be zero. This is explained by the perceived vulnerability of the child (considered too fragile at birth as described above) but also by vaccine shortages or again the "open vial policy" described above.
In short, the studies reviewed here show that vaccine uptake and compliance with the schedule in Madagascar depend on a series of interconnected factors: the relationship between the child's parents and the healthcare personnel, the practice of traditional care at birth, understanding and perceptions of immunisation and VPDs, and also the role attributed to vaccines. These studies also reveal an instrumentalisation of immunization: obtaining a health passport through immunisation is, for the parents, one of the main motivations in vaccine uptake, providing access to healthcare for the child and enhancing the caregiver-cared for relationship. (Confidence in and positive relationships with doctors are crucial factors when new mothers make a decision concerning the immunisation of their children.)
In common with numerous studies on immunisation, these anthropological surveys conducted in Madagascar revealed late uptake of vaccines or hesitancy to certain categories of vaccines, rather than complete refusal of immunisation. The researchers note that obstacles connected to availability and access to vaccines are increasing.
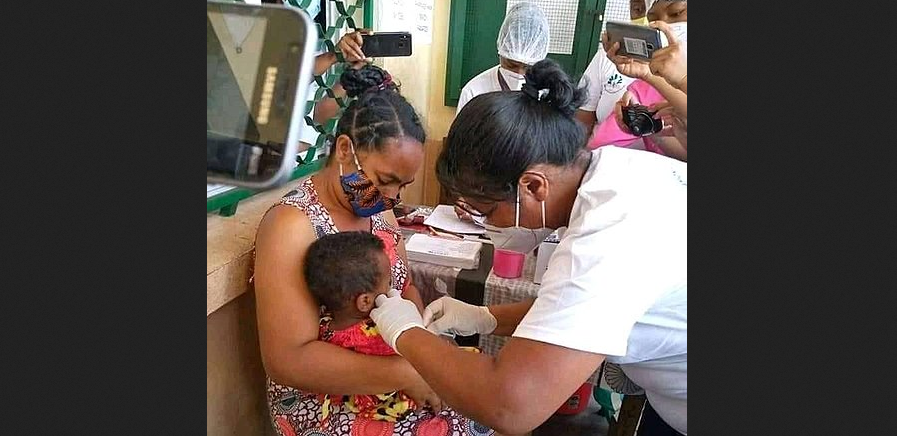
Vaccine: X Volume 15, December 2023, 100348. https://doi.org/10.1016/j.jvacx.2023.100348. Image credit: RALAIMANGA via Wikimedia (CC BY-SA 4.0)
- Log in to post comments












































