Health Care Worker Vaccination against Ebola: Vaccine Acceptance and Employment Duration in Sierra Leone
London School of Hygiene & Tropical Medicine
The potential effectiveness of prophylactic Ebola virus disease (EVD) vaccination for healthcare workers (HCWs) is partially determined by the coverage achieved during vaccination campaigns and the rate of attrition and turnover of vaccinated staff. There are currently little data on the likely acceptability of vaccination in HCWs, although there is evidence of high acceptability among community members. Thus, from June-July 2018, researchers from the London School of Hygiene & Tropical Medicine conducted a pilot survey on staff turnover and vaccine acceptance amongst 305 HCWs in Freetown and Kambia districts of Sierra Leone.
Multivariable logistic regression demonstrated which demographic and behavioural factors were associated with acceptance of a hypothetical new vaccine. The researchers quantified the duration of employment of HCWs, and used multivariable gamma regression to detect associations with duration of employment in current or any healthcare position. Finally, they simulated populations of HCWs to determine the likely future immunisation coverage amongst HCW based on estimates of vaccine acceptance and employment duration.
Most HCWs surveyed had a positive opinion of EVD vaccination (76.3%). There was no association between vaccine acceptance and experience of EVD cases, defined as knowing someone who had EVD or having worked as a HCW during the West African epidemic. Being a volunteer HCW (vs. being on the government payroll) was associated with increased vaccine acceptance. (The researchers say that further exploration of why volunteer status was associated with increased vaccine acceptance, and if there is any difference in risk or risk perception, is needed.) HCWs were found to have stable employment, with a mean duration of employment in the health sector of 10.9 years (median 8.0 years). Assuming a single vaccine campaign, with 76.3% vaccine acceptance, 100% vaccine efficacy, and no waning of vaccine-induced protection, immunisation coverage was sustained over 50% until 6 years after a vaccination campaign. If vaccine-induced immunity wanes at 10% per year, then the immunisation coverage among HCWs would fall below 50% after 3 years.
The researchers note that they surveyed HCWs in 2 areas that were affected during the 2014-16 epidemic. Therefore, it is possible that the HCWs had more experience of EVD, information, or differences in risk perception, compared with less affected areas, which could increase positive attitudes toward vaccination. Further work could survey areas with less experience of EVD to evaluate this.
There was a positive association with a moderate level of income and vaccine acceptance. Speculative reasons may be that HCWs at moderate pay have higher exposure to patients, which affects risk perception. This finding warrants further investigation to determine if it is a true association, and how risk perception relates to vaccine acceptance.
In conclusion, vaccinating HCWs against EVD could be feasible in Sierra Leone, as employment appeared stable and vaccine acceptance high. However, even with high vaccine efficacy and long-lasting immunity, repeated campaigns or vaccination at employment start may be necessary to maintain high coverage.
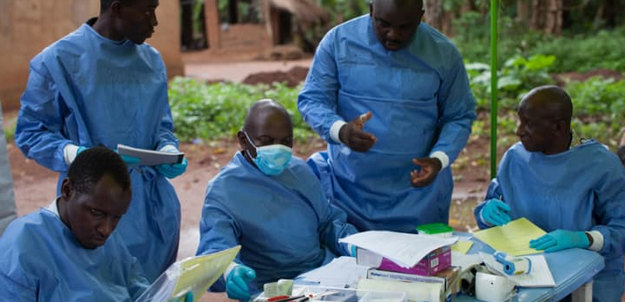
Vaccine https://doi.org/10.1016/j.vaccine.2018.12.060. Image credit: S. Hawkey / WHO
- Log in to post comments












































